The tight ligament that attaches the upper lip to the gums is called the labial frenum. The one attaching the tongue to the base of the mouth is the lingual frenum.
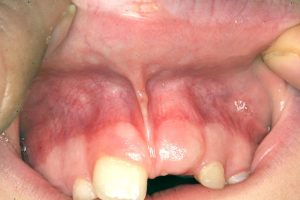
The labial frenum should be attached at least 4 mm above the gum crest of the front teeth and should not limit the lip movements Almost 10% of children will have labial frenum attachments that penetrate the papilla, or the triangular gum tissue between the central incisor teeth. These usually need intervention, as they do not resolve with age.
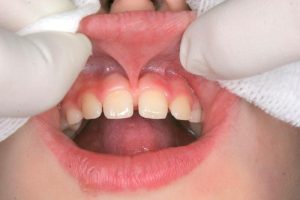
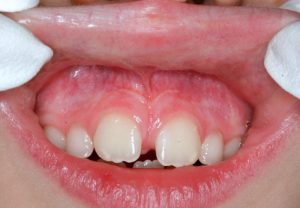
- A moderately tight labial frenum
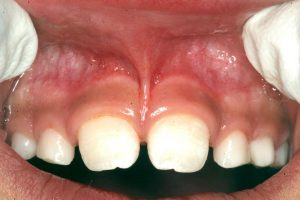
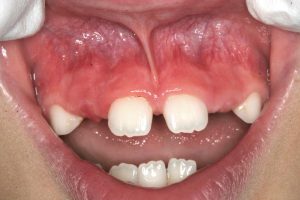
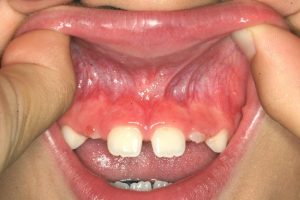
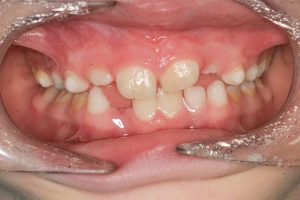
- A very tight frenum, considered the severest category
The consequences of a tight or low-attaching frenum are:
- NURSING and SUCKLING problems in infants – a serious complication, as it prevents normal latching on to the nipples, and may even produce undernourishment.
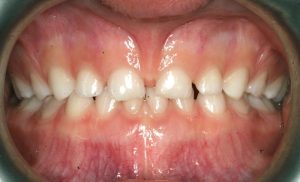
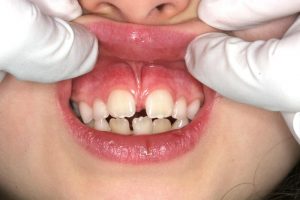
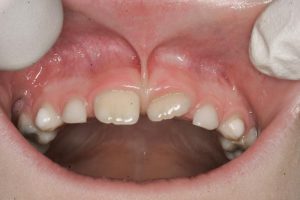
- DIASTEMA FORMATION: Due to the fibrous extension of these ligaments extending down in-between the upper front teeth, spaces between them usually do not close, and form what we know as a gap, or a diastema.
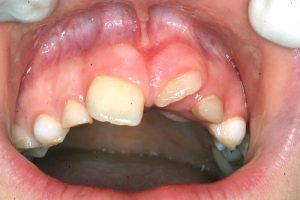
- Untreated very tight frenum causing an even bigger diastema
- in the permanent teeth as they erupt
- RECESSION: As the lip moves, it makes the frenum continually tug on the papilla (the triangular gum tissue filling the space between the upper incisors). In the future, the risk for recession and gum pockets on these teeth is higher.
- OPEN MOUTH POSTURE: The tight ligament limits lip function and prevents it from adapting with the lower lip, or forming a “lip seal”, which is an integral part of healthy nose breathing. Therefore, these children have a higher risk of open mouth posture and mouth breathing, leading to detrimental effects on jaw growth and airway development.
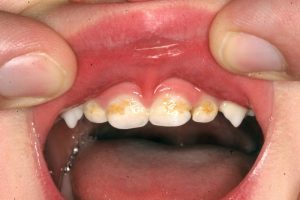
- PLAQUE, DECAY AND GINGIVITIS: Studies show that a higher lip posture due to the tight frenum is associated with more plaque retention, decay, and gum inflammation.
- A very tight labial frenum which has caused plaque accumulation and decay on the baby teeth
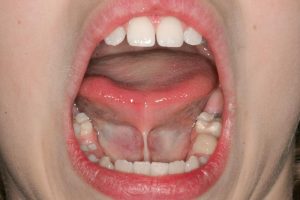
The lingual frenum should allow for free movement of the tongue, particularly in its role in swallowing, speech, and tooth and jaw development. In severe cases, it is called “ANKYLOGLOSSIA”.
- Lingual frenum
A child with a tight lingual frenum is also called “tongue tied”. One sign is a “heart-shaped” tongue as the child opens the mouth wide and extends the tip of the tongue upwards. Consequences are as follows:
- LOW TONGUE POSITION: The tongue lies lower in the mouth, therefore causing abnormal growth of the lower jaw, and insufficient growth of the upper jaw. This causes severe orthodontic problems in the future as well as a tendency for sleep apnea.
- SWALLOWING DYSFUNCTION: Upon swallowing, the tongue should rest against the upper palatal vault. If its frenum is tied, it will rest lower, and insert between the teeth. This is called tongue thrust. Orthopedic effects are insufficient growth of the upper jaw, and an open bite if there is an associated tongue thrust.
- SPEECH PROBLEMS AND LISPING: Due to improper tongue positioning, lisping is a common occurrence. Generally, the “r” cannot be rolled and some consonants cannot be properly pronounced.
TREATMENT:
Surgically releasing the frenum is called frenectomy. Conventional treatment involves a procedure where the frenum is cut with a blade or scissors, with or without sutures to reposition its attachment. Another method is using an electric device called an “electrosurge”, which is fast, but painful, and it creates a zone of “burnt” tissue which not only heals slow, but heals with more scarring, therefore defeating the purpose.
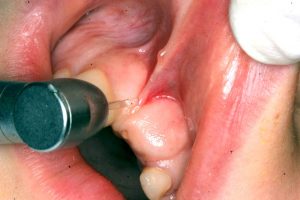
Today, in some offices, including ours, we employ a procedure called “laser frenectomy” in which the waterlase is used to zap the frenum with laser pulse, gently severing it from its attachment. A few drops of anesthetic makes the area numb enough so even a 6-year old can tolerate it.
- A young boy with a tight frenum as well as a trapped central incisor which failed to erupt
- The waterlase is being used to perform not only the frenectomy, but also to remove the thick gum covering the trapped tooth
- The follow-up visit a month later reveals perfect healing and the incisor already breaking through
Advantages:
- Healing time is reduced drastically. Full healing with new skin is evident within 10 days.
- The actual procedure takes 3-5 minutes
- There is no burning or cutting, therefore the laser frenectomy can be performed wider and deeper, thus improving the final results. The new frenum attachment is at least 5 mm higher up, clearing the gums and releasing the tongue or the lip respectively.
- In 3 weeks the labial frenum is perfectly healed and now attaches 5 mm higher than before
AFTER-CARE
Homeopathic Arnica and Hypericum in 30C potency is given half an hour apart, three times a day for three days. The area is gently dabbed with gauze soaked in a calendula/glycerin tincture (non-alcoholic). Otherwise, rinse with a strong sea-salt solution. For the next two weeks post-operatively the child and parents are instructed to perform, any chance they get, stretching exercises on the lip (grabbing the lip and moving it in all directions) to allow the re-attachment of the fibers as far away from the gums as possible.
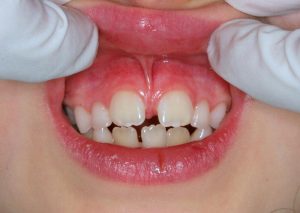
- A moderate labial frenum attaching to the papilla and causing a diastema (space between teeth)
- The appearance of the area less than a week after laser frenectomy
- The area fully healed after three weeks
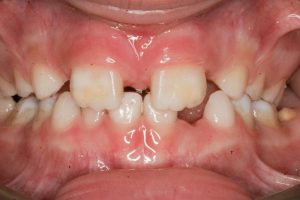
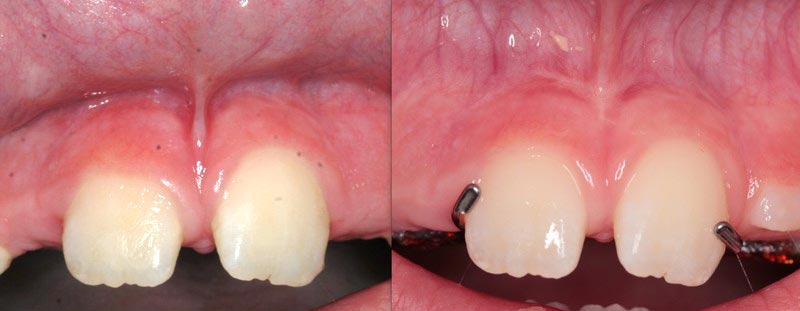
- A tight frenum before treatment
- The frenum after laser frenectomy
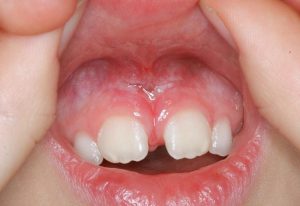
- A tight labial frenum
- A tight frenum before treatment
- The frenum after laser frenectomy

What do you suggest is the best age to have the frenectomy done?
Another excellent article, I would very much enjoy getting copies to hand out to inform and educate my patients. Thank you again for great topics
Do you have a brochure that explains the frenectomy to distribute?
Hi Amanda, unfortunately not, but you can just pass on our web page. Thank you!
At what age is the surgery recommended in a child? Thank you